Pregnancy can have a number of effects on a woman’s feet, including:
- Swelling: Pregnant women may experience swelling in their feet and ankles due to the increased pressure on the blood vessels and the accumulation of fluid in the tissues.
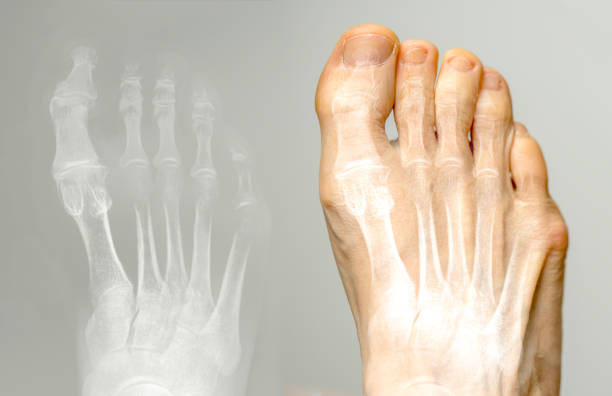
- Flat feet: The increased weight and changes in hormones during pregnancy can cause the arches of the feet to flatten, leading to pain and discomfort.
- Varicose veins: The pressure on the blood vessels in the legs during pregnancy can cause varicose veins to develop, which can be painful and unsightly.
- Numbness and tingling: Some women may experience numbness and tingling in their feet due to the compression of nerves in the lower back and legs.
- Changes in shoe size: The swelling and changes in foot structure during pregnancy can cause a woman’s shoe size to increase temporarily.
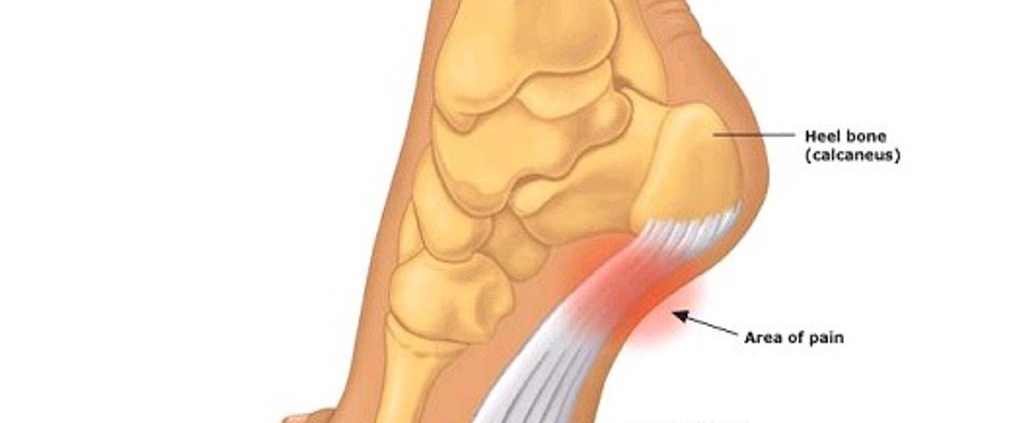
- Plantar fasciitis: The added weight and changes in gait during pregnancy can also contribute to the development of plantar fasciitis, a condition that causes pain in the heel and bottom of the foot.
To help manage these effects on the feet during pregnancy, women can take several steps, such as wearing comfortable and supportive shoes, elevating their feet whenever possible, doing regular exercises to improve foot strength and flexibility, and wearing compression stockings to improve blood flow. It’s also important to discuss any concerns or symptoms with a healthcare provider to ensure proper diagnosis and treatment.